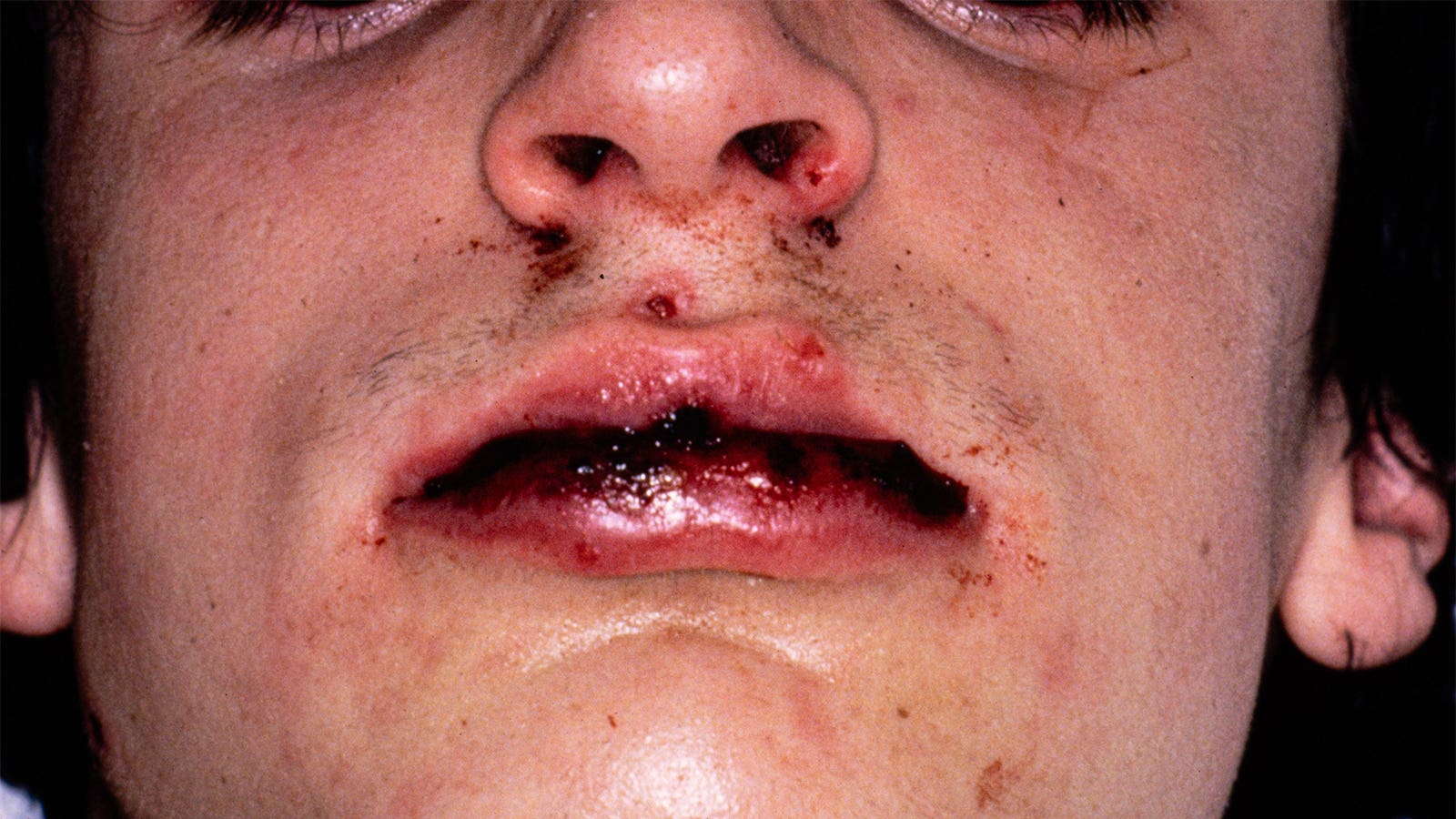
Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) represent severe allergic skin reactions triggered by medications, often resulting in profound and enduring effects on patients’ vision, daily functioning, and overall well-being.
In a detailed qualitative investigation, fewer than half of the 29 survivors interviewed indicated they received straightforward instructions upon leaving the hospital. Moreover, 13 participants highlighted the immense stress caused by having to independently manage their recovery without proper guidance.
The study’s authors emphasized the urgent necessity for improved care coordination between patients and their primary doctors, enhanced education for both healthcare providers and patients, and dedicated mental health resources.
Persistent Challenges After Hospital Release
Individuals who have endured SJS or TEN shared accounts of ongoing complications coupled with woefully inadequate education and assistance following their hospital stay, according to findings from a comprehensive survey-based analysis.
Just under 50% of the 29 study participants reported obtaining explicit directions post-discharge. Thirteen individuals specifically pointed out that figuring out their care pathway on their own, absent any professional direction, generated considerable emotional strain. These insights were detailed by Elizabeth J. Phillips, MD, from the Center for Drug Safety and Immunology at Vanderbilt University Medical Center in Nashville, Tennessee, along with her research team, in a publication within JAMA Dermatology.
Outpatient clinicians whom these survivors consulted often demonstrated limited expertise and skills in handling SJS/TEN cases. This knowledge gap exacerbated feelings of worry, emotional turmoil, and skepticism toward the medical system. Consequently, many survivors shunned essential treatments and turned to online sources for advice.
The research team underscored that these observations reveal a critical requirement for structured post-discharge collaboration between patients and their main healthcare providers, incorporating mental health services. Such arrangements ought to be established before patients exit the hospital to guarantee sufficient resources and the best possible recovery results. Furthermore, it is vital for medical professionals and investigators to deepen their comprehension of the prolonged effects of SJS/TEN and to refine existing discharge protocols and educational materials for affected individuals and their loved ones.
Understanding SJS/TEN and Its Broader Implications
SJS and TEN qualify as intense cutaneous hypersensitivity responses induced by drugs—commonly initiated by agents such as sulfa-based antibiotics or anticonvulsant medications. These conditions impact between 1 and 5 individuals per million annually, potentially causing vision loss, total blindness, and sustained disruptions to physical capabilities and life satisfaction.
Even within the disjointed landscape of the American healthcare framework, organized multidisciplinary assistance remains achievable, as evidenced by management strategies for other uncommon disorders like spina bifida, the researchers contended. At the very least, follow-up care for SJS/TEN patients should encompass mental health evaluations, dermatological consultations, and ophthalmological assessments.
Insights from the SJS Survivors Study
This research drew from the community-oriented SJS Survivors Study, featuring in-depth, semi-structured telephone interviews with 29 U.S.-based participants about their post-hospital experiences with SJS/TEN. Conducted between July 2021 and August 2023, these discussions involved an interviewer with no previous connections to the participants.
The interviewees’ ages spanned from 26 to 76 years, averaging 46 years old, with 66% female and 69% identifying as white. The majority (41%) were interviewed within five years of their reaction, though the median timeframe was six years, extending up to 35 years in some cases. Approximately 75% had experienced severe manifestations involving at least 10% of their body surface area.
Emotional and Physical Struggles in the Initial Months
Reflecting on the first six months after discharge, participants conveyed a profound sense of losing the structured support available during their hospitalization. They felt profoundly alone, lacking resources to comprehend the enduring repercussions of SJS/TEN on their personal lives and those of their families.
Survivors recounted enduring physical ailments such as chronic skin problems, severe visual deficits leading to blindness, and diminished independence in daily activities. Psychologically, they grappled with heightened anxiety, compulsive thoughts, traumatic recollections, and depressive episodes during this vulnerable phase. Five individuals received formal PTSD diagnoses, while ten others exhibited notable symptoms consistent with the condition. Several advocated for compulsory mental health referrals and interventions at the time of discharge.
One participant articulated: “I don’t believe it was my responsibility to push for mental health care. I wasn’t required to fight for an eye exam after nearly losing my sight, so why should mental health be any different? It ought to have been automatically scheduled for me.”
A recurring theme was the frustration and isolation stemming from independently coordinating post-hospital treatment without adequate support.
Gaps in Education and Physician Awareness
Participants frequently noted the absence of proactive educational efforts and discharge planning tailored to their diagnosis. The researchers observed that physicians’ unfamiliarity with SJS/TEN was especially prominent, prompting survivors to seek internet-based information rather than physician-led advice. Distrust in medical professionals emerged as a frequent issue among this group.
Study Limitations and Paths Forward
Among the study’s constraints were the underrepresentation of males and individuals from racial and ethnic minority backgrounds, alongside possible selection bias favoring those with more severe SJS/TEN episodes.
Looking ahead, Phillips and her colleagues recommended that subsequent research assess standard discharge teaching and procedures, with a focus on incorporating details about long-term consequences, post-discharge mental health monitoring by qualified psychologists, and connections to peer support networks.